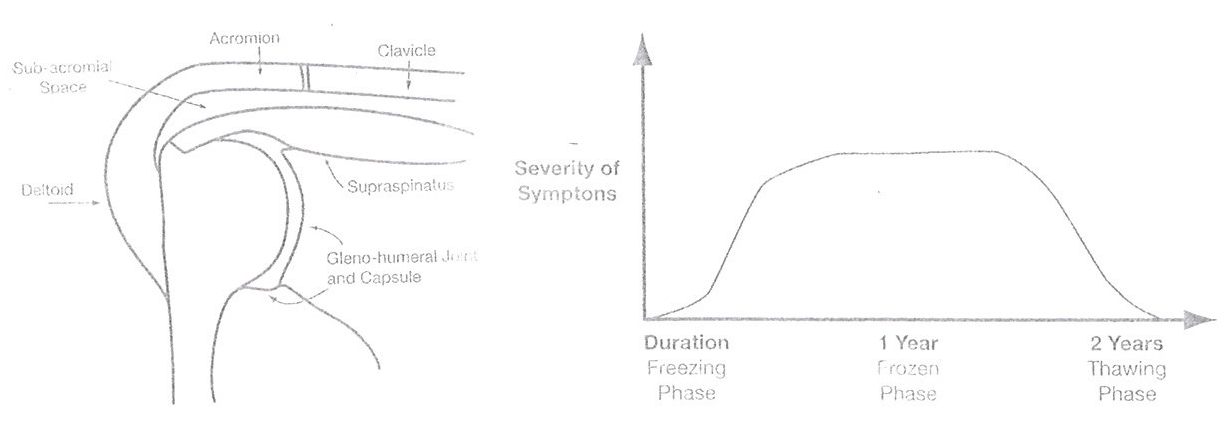
Symptoms and Causes of Frozen Shoulder
Frozen shoulder is a condition, which results in pain and stiffness of the shoulder in all directions of movement. It has also been known by several other names such as “adhesive capsulitis” or “glenohumeral capsulitis”. This reflects the relatively poorly understood nature of this condition.
The glenohumeral or shoulder joint has a lining called synovium and a casing called the capsule. These structures become inflamed and although inflammation is a normal physiological process, the intensity and duration of the inflammation is greatly increased. This inflammatory process results in a painful joint and also leads to progressive stiffness of the joint, which may become quite severe. The capsule of the joint becomes stiff and thickened and the amount of joint lubricating fluid is decreased.
Although the cause is not known, it is not arthritis. We do know that the condition occurs more frequently and with greater severity in people with diabetes. Generally, the condition tends to affect women in their middle age, although men may also be affected. It may be triggered by a relatively minor traumatic incident such as a sudden yank or fall on the shoulder. Often no particular initiating event can be found.
The condition generally affects the glenohumeral joint and it may have effects in the subacromial part of the joint, particularly in the early stages of the condition and resemble “impingement syndrome” or “rotator cuff tendonitis”. This may have led to difficulty in establishing the diagnosis.
Duration and Intensity of Frozen Shoulder
Frozen shoulder is generally regarded as being a self-limiting condition. This implies that after a period of time, the condition will gradually resolve of its own accord. The duration and intensity of the condition between individuals can vary enormously. It is not uncommon for the condition to continue for up to 18 or 24 months. The most usual course of events is for complete recovery. 7%-10% of individuals may have some eventual restriction of movement and this again is much more frequent in diabetics.
Symptoms may be quite severe and disabling. The pain is usually felt throughout the day and is often worse at night leading to loss of sleep. The pain is minimal when the arm is moved through a range of movement and is limited by stiffness, if one attempts to move the arm beyond the limits of the stiffness then the pain is usually intensified. The restriction of movement may be asymmetric, ie it may be greater in some direction than others.
Treatment for Frozen Shoulder
Many frozen shoulder treatment options have been used over the years. There is no absolute cure. The intensity and duration of the symptoms may be influenced by certain therapeutic manoeuvres. When the diagnosis is first made we generally recommend a course of gentle stretching exercises and usually inject the glenohumeral joint (and occasionally the subacromial joint) with an anti-inflammatory agent and local anaesthetic in an attempt to reduce inflammation. This may be repeated two or three times and usually results in a significant improvement in the degree of pain and therefore, may make the arm more functional.
Occasionally if the duration of the symptoms is prolonged, the stiffness severe or the patient is a diabetic then consideration may be given to a surgical release of the lining of the joint. This may either be performed by manipulation of the shoulder under anaesthetic or by surgically releasing the capsule using the arthroscope and a cutting electrocautery knife.
Doctors Who Specialise in Shoulder Surgery
It is important to remember that the overwhelming number of patients with the condition will eventually resolve on its own accord and, therefore, will not require surgery. It is a particularly frustrating condition, which requires considerable patience. Recurrence is unusual, but the opposite shoulder is not infrequently affected at a later date.
It is however important to consult and seek help from doctors who specialise in shoulder surgery when you feel that you need an intervention.